What is sickle cell disease?
Sickle cell disease affects the hemoglobin within your red blood cells. A genetic mutation causes abnormal hemoglobin to clump together, causing the red blood cells to turn sickle shaped. These sickle-shaped cells cause blockages in your blood flow, which can lead to anemia, pain, infections and severe complications.
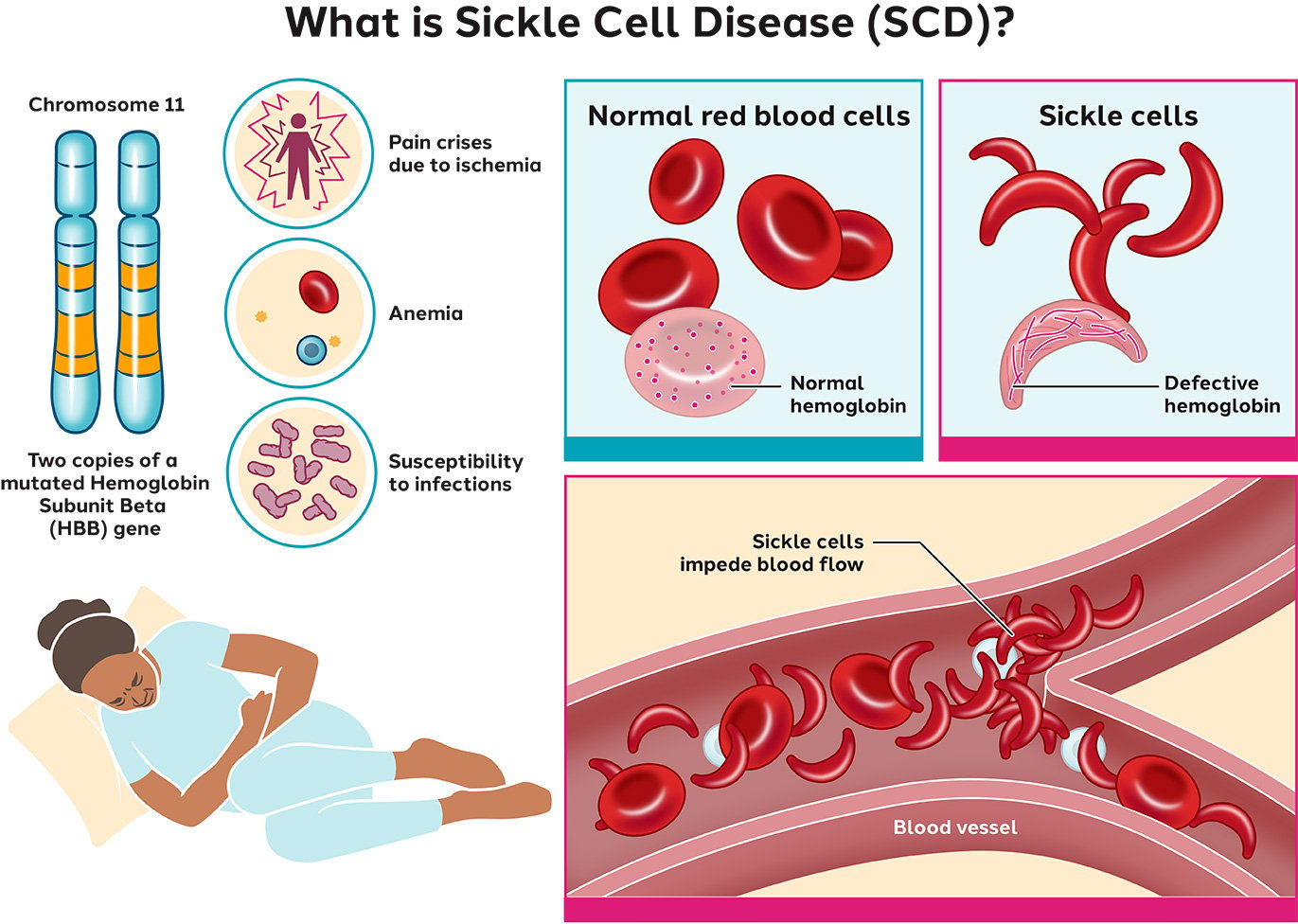
What is sickle cell disease?
Sickle cell disease (SCD) is the most common inherited blood disorder that affects your red blood cells. In SCD, a protein called hemoglobin, located within red blood cells, is abnormal. Hemoglobin is important. It’s the molecule that carries oxygen in your blood and throughout your body.
Normal red blood cells are round and flexible. This allows them to move easily through small blood vessels (capillaries) in your body to deliver oxygen to your organs and tissues. In SCD, there’s an abnormal form of hemoglobin called hemoglobin S. This changes the shape of the red blood cell to a crescent shape and causes red blood cells to become rigid, lack flexibility and stick together. This can block blood flow, preventing oxygen from getting to the vital organs and tissues throughout your body. It can lead to serious complications including pain, infections, and organ damage and failure. Additionally, sickle-shaped cells don’t last as long as normal-shaped red blood cells, causing a constant shortage of red blood cells and leading to anemia. Sickle cell disease is a lifelong condition. But there are treatment options that can reduce your symptoms and prolong your life.
Types of sickle cell disease
There are several types of sickle cell disease. The different types depend on the genes a person inherits from their parents.
Hemoglobin SS (HbSS)
HbSS is a severe form, affecting 65% of people who have SCD. People with this form inherited one gene encoded with hemoglobin S from each parent. Most or all of your hemoglobin is abnormal, causing chronic anemia.
Hemoglobin SC (HbSC)
HbSC is a mild to moderate form that affects about 25% of people with the disease. People with this form inherited a hemoglobin S gene from one parent. They inherited another abnormal type — hemoglobin C — from their other parent.
Hemoglobin (HbS) beta thalassemia
People with this form inherited a hemoglobin S gene from one parent. They inherited an abnormal type called beta thalassemia from their other parent. There are two subtypes:
- “Plus” (HbS beta +): This subtype affects about 8% of people with SCD and tends to be more mild.
- “Zero” (HbS beta 0): This subtype affects about 2% of people with SCD and is more severe, similar to hemoglobin SS disease.
There are other, more rare forms, including hemoglobin SD (HbSD), hemoglobin SE (HbSE) and hemoglobin SO (HbSO). People with one of these forms inherited one hemoglobin S gene and one gene that encodes with another abnormal gene (D, E or O).
What’s the difference between sickle cell anemia and sickle cell disease?
Sickle cell disease is an umbrella term for the many different types of sickle cell disorders. Healthcare providers reserve the term “sickle cell anemia” for the types of SCD that cause the most severe anemia. These types are hemoglobin SS and hemoglobin beta zero thalassemia.
Sickle cell trait vs. disease
People who have sickle cell trait inherited a hemoglobin S gene from only one parent. They inherited a normal gene from their other parent. People with sickle cell trait typically don’t have any symptoms of sickle cell disease. But ongoing research may show that these people may have symptoms. They can pass on the abnormal gene to their own children.
Rarely, severe dehydration and intense physical activity can lead to serious health issues in people with sickle cell trait.
How common is sickle cell disease?
Researchers estimate sickle cell disease affects about 100,000 Americans. The disorder occurs in about 1 in every 365 Black births. It occurs in about 1 in every 16,300 Hispanic American births. About 1 in every 12 people of Black or African descent carries the sickle cell trait.
Symptoms and Causes
What causes sickle cell disease?
A genetic mutation in the HBB gene causes sickle cell disease. The HBB gene is responsible for making a part of the hemoglobin. People with SCD received two mutated HBB genes coded for abnormal hemoglobin — one from each parent.
People inherit SCD in an autosomal recessive manner. This means each parent of a child with SCD carries one copy of the mutated gene, but they typically don’t show signs and symptoms of the condition.
Who’s at risk of developing sickle cell disease (SCD)?
Certain groups of people are more likely to develop SCD, including:
- People of African descent, including African Americans.
- Hispanic Americans from South America and Central America.
- People of Mediterranean, Middle Eastern, Indian and Asian descent.
What are the symptoms of sickle cell disease?
Sickle cell disease symptoms begin to show when a child is about 5 to 6 months old. Signs and symptoms of SCD vary from person to person. Some people have mild symptoms, while others develop more serious complications. Sickle cell disease symptoms include:
- Frequent pain episodes.
- Anemia, causing fatigue, paleness and weakness.
- Jaundice (yellowing of their skin and the whites of their eyes).
- Painful swelling of their hands and feet.
What are the complications of this condition?
Sickle cell disease can affect many parts of your body. Some of the effects are acute (they start suddenly) and some are chronic (they last for a long time). Sickle cell complications begin early and continue throughout your life.
Pain
Pain is the most common complication of sickle cell disease. Sickled cells passing through blood vessels can get stuck and block blood flow, which causes pain. You may have an acute pain crisis, which is also called a sickle cell crisis, vaso-occlusive crisis (VOC) or vaso-occlusive episode (VOE). These pain crises may be mild or severe and can start suddenly and last for any length of time. Pain crises most often affect your chest, back, legs and arms. You might also have chronic pain, which is when pain lasts longer than six months.
Anemia
Red blood cells die early with sickle cell disease, which can lead to anemia. Anemia occurs when you don’t have enough healthy red blood cells to carry oxygen throughout your body. Anemia can cause severe fatigue, along with jaundice, irritability, dizziness and lightheadedness.
Acute chest syndrome
Acute chest syndrome is a life-threatening medical emergency. It can cause lung injury, difficulty breathing and low oxygen to the rest of your body. This complication of SCD occurs when sickled cells block blood and oxygen from reaching your lungs.
Blood clots
Sickled cells make it more likely for blood to clot. This increases your chances of developing a blood clot in a deep vein (deep vein thrombosis, or DVT). A DVT can break off and travel to your lungs (pulmonary embolism, or PE).
Stroke
When sickled cells get stuck in a blood vessel, it blocks blood flow to your brain. This makes it harder for your brain to get the oxygen it needs to work correctly. This can lead to a stroke. About 10% of people with SCD will have a symptomatic (clinical) stroke. Strokes are most common in people with sickle cell anemia.
Vision problems
Sickled cells can block blood flow in the blood vessels in your eyes. This blockage occurs most often in the retina of your eye. You may not have any symptoms and then suddenly have vision loss, which can lead to permanent blindness.
Priapism
Sickled cells in your penis can cause a persistent, painful erection (priapism). In addition to causing pain, priapism can cause permanent damage and erectile dysfunction. A prolonged priapism (lasting longer than four hours) is a medical emergency.
Organ damage and failure
People with sickle cell disease are at risk for problems related to their heart, lung, kidneys and other organs. This is because blood and oxygen aren’t reaching them. SCD can lead to multi-organ failure.
Does sickle cell trait or sickle cell disease affect pregnancy?
Many people with sickle cell disease have healthy pregnancies, but the risks are higher. SCD can increase the risk of high blood pressure, blood clots, miscarriage, low birth weight and premature birth.
Diagnosis and Tests
How is sickle cell disease diagnosed?
In the United States, hospitals test all babies for sickle cell disease as part of routine newborn screenings. This test pricks your baby’s heel to get a sample of their blood. It checks for various other conditions, as well. Your child’s healthcare provider will obtain a hemoglobin electrophoresis to confirm the diagnosis.
Your healthcare provider can also diagnose sickle cell disease before your baby is born using prenatal testing. These tests include chorionic villus sampling and amniocentesis.
Management and Treatment
Is there a cure for sickle cell disease?
A bone marrow transplant (stem cell transplant) can cure sickle cell disease. The transplant requires a donor who’s a healthy, genetic match, such as a sibling. In this procedure, you receive healthy marrow from the donor. However, only about 18% of people with SCD have a compatible donor. In addition, there are risks and complications involved with a transplant. Your healthcare provider will discuss these issues with you.
What is the treatment for sickle cell disease?
Sickle cell disease treatment includes medications, transfusions, blood and marrow transplant and gene therapy. Sickle cell disease treatment may begin with antibiotics. Newborns with severe SCD will receive antibiotics twice a day until they’re 5 years old to prevent infection.
Other sickle cell disease medications
Most people with SCD use medications to make their disease less severe and treat symptoms. These medications include:
- Voxelotor: Voxelotor can prevent red blood cells from sickling and binding together. It may reduce the destruction of some red blood cells, which improves blood flow to your organs and lowers your risk for anemia.
- Crizanlizumab: This medicine helps prevent sickled red blood cells from sticking to your blood vessel walls. This can improve blood flow and reduce inflammation and pain crises.
- Hydroxyurea: Hydroxyurea can reduce or prevent several complications of SCD. This includes frequent pain crises, acute chest syndrome and severe anemia.
- L-glutamine: This medication is a pain reliever that can help reduce the number of pain crises you have. Other pain medication options include nonsteroidal anti-inflammatory drugs (NSAIDs) and opiates.
Transfusions
Your healthcare provider may recommend certain transfusions to treat and prevent SCD complications. These transfusions may include:
- Acute transfusions: Acute blood transfusions can help treat complications that cause severe anemia. Your provider may also use an acute transfusion to treat crises. This includes strokes, acute chest syndrome and organ failure.
- Red blood cell transfusions: Red blood cell transfusions can help increase the number of red blood cells in your body and provide normal, non-sickled red blood cells.
Stem cell transplant (also known as blood or marrow transplant)
A stem cell transplant can cure SCD. Sometimes called blood or marrow transplant, SCT requires a donor who’s a good match, like a sibling, and ongoing studies are looking to optimize the transplant from alternative donors, such as birthing parents or siblings who only half-matched. Your healthcare provider will discuss the risks and benefits of this treatment in your specific case.
Gene therapy
Researchers are currently testing gene therapy to treat SCD. This calls for correcting an abnormal hemoglobin gene or putting a normal hemoglobin gene into a person’s stem cells. There’s promising early data and the hope is that gene therapy might one day be a routine treatment for SCD.
Prevention
Can this be prevented?
You can’t prevent sickle cell disease because it’s a genetic condition. If you’re pregnant, consider talking to your provider about genetic testing or genetic counseling.
Outlook / Prognosis
What can I expect if I have sickle cell disease?
People with sickle cell disease have a reduced life expectancy. New treatments for SCD are improving life expectancy and quality of life. People with sickle cell disease can survive beyond their 50s with optimal management of the disease.
Living With
How do I take care of my child if they have sickle cell disease?
If your child has sickle cell disease, there are many things you can do to help manage their condition:
- Take your child to see their healthcare provider regularly.
- Make sure your child gets all their recommended vaccines.
- Help your child get regular exercise and eat a heart-healthy diet.
- During a pain crisis, have your child drink lots of fluids and take a nonsteroidal anti-inflammatory drug (NSAID).
- If you can’t manage their pain at home, take them to the hospital for stronger pain medication.
When should I go to the ER?
Sickle cell disease can lead to many different life-threatening complications. If you or your child experiences any of the following symptoms of complications, call 911 or go to the nearest emergency room:
- Severe pain.
- Symptoms of severe anemia, including fatigue, dizziness and shortness of breath.
- Fever of 101.3 degrees Fahrenheit (38.5 degrees Celsius).
- Vision problems.
- Difficulty breathing.
- Erection lasting for four or more hours.
- Symptoms of acute chest syndrome, including chest pain, coughing and fever.
- Symptoms of stroke, including sudden weakness, numbness on one side of your body and confusion.
Additional Common Questions
Why does sickle cell disease cause pain?
Sickled red blood cells are C-shaped and look kind of like crescent moons. When they travel through your blood vessels, they can get stuck and clog up the flow of blood, causing pain.
Is sickle cell an autoimmune disease?
No. Sickle cell disease shares some characteristics with autoimmune diseases. But healthcare providers don’t consider SCD an autoimmune disorder. They consider SCD a genetic condition.
A note from Cleveland Clinic
Sickle cell disease is a lifelong condition. While there’s a cure available, stem cell transplants aren’t always available and come with many risks. However, early diagnosis and treatment can help reduce your symptoms and chances of complications. With ongoing care, you can go on to lead a full, active life.